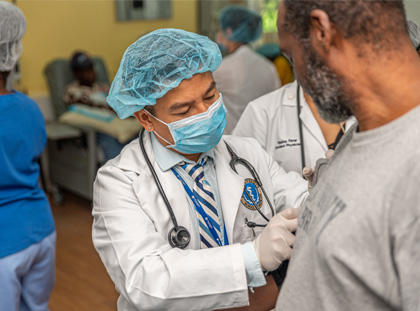
A hospitalist is a doctor who works exclusively in a hospital. As an internal medicine hospitalist—the most common type—you will provide general medical care to hospitalized patients. Aside from clinical care, hospitalists also teach, do research, and work to improve hospital and healthcare system performance. If you are considering a career as a hospitalist, ask yourself these questions:
- Are you fascinated by the fast-pace hospital environment?
- Do you want to provide a wide range of care to a wide range of patients?
- Do you want a field that offers professional challenges and specialized options?
- Are you passionate about helping people with chronic health problems?
- Do you want a career in one of the newest and most in-demand fields of medicine?
- Do you want to do research, visit patients in wards, and work in the intensive care unit all in one day?
If your answer to these questions is “yes,” then a career as a hospitalist may be the right path for you.
What Does a Hospitalist Do?
Compared to other specializations, hospital medicine—the practice of medicine specifically in a hospital—is practically brand new. The term hospitalist was coined only in 1996, and the Society of Hospital Medicine was formed a year later in 1997. Many hospital patients may be surprised to learn that the doctor caring for them is most likely a hospitalist.
The need for such a specialty emerged from increasingly complex hospital patient cases. These cases required physicians who could dedicate their time to hospital patients rather than doctors who might visit only when not managing ambulatory care or other obligations. This need for easier accessibility combined with desires for greater efficiency and lower hospital costs to produce the new field of hospital medicine.
Hospitalists specialize on a site of care—the hospital—rather than an organ—such as a pulmonologist—a disease—such as an oncologist—or a patient’s age—such as a pediatrician. Pulmonological, oncological, and pediatric hospitalists exist, but most hospitalists specialize in family or internal medicine.
Hospitalists can serve patients in a wide variety of ways, from the emergency room to critical care to post-operative or post-acute care. Hospitalists may also perform diagnostic exams, procedures, or tests. Hospitalists may become experts in certain types of injuries or maladies as they treat similar conditions over and again.
Because hospitalists see a wide number of patients, and most only for short periods, they do not develop long-term patient relationships the way primary physicians do. Hospitalists do, however, communicate with the patients as well as their families, often delivering anxiously awaited news.
Aside from general medical care, hospitalists have further duties that many other doctors do not. A hospitalist is well-versed in hospital policy and may serve on various committees. Hospitalists may take on leadership roles or be involved in increasing efficiency and reducing medical errors or improving overall safety and quality of care. Responsibilities also include preparing patients to leave the hospital and reducing the length of stay: shorter stays reduce hospital costs.
Hospitalists treat injuries and illnesses that are serious enough to bring people to the hospital. They commonly deal with:
- Bone fractures
- Burns
- Contusions
- Head trauma
- Illnesses
- Infections
- Joint sprains
- Poisoning
- Pre- and post-operative care
- Wounds
Many hospitalists are also active in academic circles and participate in conferences and publications dedicated to advancing medical knowledge and therapeutic options.
HOW TO BECOME A HOSPITALIST
To become a hospitalist, you must first become a physician by graduating from an accredited medical school*—such as Ross University School of Medicine (RUSM). The steps to a medical degree at RUSM, which is located on the Caribbean island of Barbados, are the same as at United States-based schools: two years of medical science classes and two years of hands-on clinical training. For RUSM students, the medical sciences curriculum is completed on the Barbados campus; the clinical training can be completed at affiliated teaching hospitals in the United States.
During clinical training, RUSM students complete core rotations in internal medicine, surgery, pediatrics, family medicine, obstetrics/ gynecology, and psychiatry. Each individual student, then, selects from among 40 specialty elective clerkships to fulfill their remaining clinical requirements.
During the fourth and final year of medical school, students prepare for the next step in their medical education: residency. At RUSM, the Office of Career Advisement (OCA) helps students determine which residency specialty suits them best. The OCA then helps students negotiate the National Resident Matching Program® (NRMP®)—a placement system which medical students who want to obtain licensure in the United States use to “match” with a medical residency. Residencies are required to become a licensed physician, and they last from three to eight years. Most hospitalists complete a residency in emergency, family, or internal medicine, and then do a one-year fellowship in hospital medicine.
In 2021, RUSM had a first-time residency attainment rate of 92 percent for 2020-2021 graduates, a match percentage rate comparable with the overall match rate (93 percent) for medical schools in the United States. In recent years, RUSM MD’s have matched with hundreds of emergency, family, and internal medicine residencies at prestigious hospitals across the United States. These include the Eisenhower Medical Center in California; the JFK Medical Center in New Jersey; Medstar Washington Hospital Center in the District of Columbia; and the University of Chicago Medical Center in Illinois.
Board certification in hospital medicine is generally not required to be a hospitalist, but certification is offered by the American Board of Hospital Medicine. The American Board of Internal Medicine® certifies doctors in “Internal Medicine with a Focused Practice in Hospital Medicine,” and the American Board of Family Medicine offers a “Designation of Focused Practice in Hospital Medicine” certification.
MEET A HOSPITALIST
Melissa A. Woo, MD, a 2016 RUSM graduate, is an internal medicine hospitalist at Cleveland Clinic Florida in the Miami-Fort Lauderdale metro area. We asked Dr. Woo to describe the role of a hospitalist.
Q: Why did you decide to go into internal—and then hospital—medicine?
A: When I was a third year medical student I came to learn that I loved non-surgical specialties, and I wanted to work with adults. The third year core internal medicine rotation at Cleveland Clinic Florida (CCF) showed me the wide variety of cases, both bread and butter and rare cases, that one can come across in Internal Medicine, and in a very academic setting. I realized that I really enjoyed being able to manage all of the organ systems, so I knew that internal medicine would be the right fit for me. As time went on during residency training at CCF, I fell in love with my hospital rotations, so I knew becoming a hospitalist was the right path for me. I loved CCF so much from my time as a medical student and resident, and I am so thankful that I have been able to stay on as a staff hospitalist!
Q: Any advice to medical students considering the specialty?
A: My advice is to keep an open mind. When I was a third year medical student at RUSM, it became quite clear during my rotations that I was falling in love with internal medicine. However I really gave my all with each core rotation. When I started my journey at RUSM I did not know what specialty was for me, but I kept in very close touch with the RUSM OCA who helped guide me in the decision making process of choosing a specialty, and they were a hugely important part of my journey; it is a very personal decision and can be difficult to choose a specialty. Choose 4th year electives that will help to show you what it will be like being an internist in the clinic versus the hospital, as well as what it would be like to be a different kind of internal medicine sub-specialist (i.e., cardiologist, gastroenterologist, etc.).
Q: What’s the most rewarding part of your job?
A: I love the pace of hospital medicine and I love being able to see real-time results. Although I only see hospitalized patients for a short period of time while in the hospital, I enjoy forming connections and relationships with my patients each day and seeing them recover. It is a wonderful and emotional feeling for me and my patients to experience their recovery together and to be their cheerleader, resource, and support system through difficult medical decision-making.
If you want to become a doctor, and a career in hospital medicine appeals to you, learn more about the RUSM MD Program and investigate the Office of Career Advisement. When you’re ready, take the next step on your path to a specialization in hospital medicine: apply for admission to Ross University School of Medicine.
Why Do Hospitals Use Hospitalists?
Unlike primary physicians, hospitalists do not have office hours and usually work varying shifts. Most time is spent caring for patients, but many hours are spent doing laboratory work or performing procedures. Meetings and administration tasks absorb a lot of time, and hours are also spent consulting with specialists and nurses, doing research, studying, and teaching. Many hospitalists work 12-hour shifts and many work time blocks—such as seven days on, seven days off. Unlike many doctors, most hospitalists are not on-call during their time away from work. Hospitalists can have a great impact on a patient’s hospital stay as well as the overall function of their hospital.
Demand for Hospitalists
Hospital medicine is currently the fastest growing medical specialty in the United States. Many internal medicine physicians are choosing to become a hospitalist, as opposed to a primary care physician. With the number of people being hospitalized increasing, patients require a physician that can provide consistent care and help them navigate through their hospital stay.
In 2020, hospitalists were on the front line during the COVID-19 pandemic, and hospitals were often hard-pressed to staff the constant hospitalist rotations. In many cases, hospitalists were pressed into unfamiliar duties as COVID-19 patients overwhelmed hospitals worldwide. Many hospitalists are now experts in caring for people with COVID-19.
Unlike physicians in other medical specialties, hospitalists are not an aging population. According to an annual survey conducted by Today's Hospitalist, about 28% of hospitalists are between ages 36 and 40, while about 20% are between 41 and 45. This is largely due to the fact that hospital medicine has only been around for two decades.
The Ross University School of Medicine has a strong history of placing graduating students in internal medicine residencies. In 2020, RUSM’s 2019-2020 first-time residency attainment rate was 95 percent. Take the next step toward becoming a hospitalist: apply for admission to RUSM.
Related resources: